Healthy Skepticism International News
January 2001
Scepticism and beliefs about new drugs
January/June 2001 Vol 19 No 1/6 Dr Peter Mansfield GP (Aldinga Beach, South Australia), Consultant on marketing and appropriate use of therapies and Director of MaLAM (Medical Lobby for Appropriate Marketing) Associate Professor Joel Lexchin, Emergency Medicine/Primary Care, Toronto General Hospital and Author of "Drugs of Choice" for Canadian GPs This edition was published on paper in three parts. It provides our subscribers with a copy of the feedback written by HealthySkepticism.org for Australian general practitioners who participated in a case study based educational exercise commissioned by the Australian National Prescribing Service (NPS). For further information about the NPS please visit: www.nps.org.auScenario
You are visited by Mrs Parker an overweight 50 year old woman with mild hypertension and mildly elevated cholesterol levels but no other risk factors. Her only symptoms are insomnia and crying as she thinks her life is worthless now that her children have left home. She is also anxious about her son’s wedding in 6 months because she has always felt overwhelmed by big parties.Introduction
This cases study was released in December 1999 but we were still receiving responses in September 2000 when this report was written. The case scenario was designed to reflect the uncertainty seen in real life in general practice so the information was complex, ambiguous and incomplete. Consequently, different GPs may have good reasons for interpreting the scenario and the questions differently. For that reason there are no right answers. However we have provided our "recommended answers" with very brief comments based on a sceptical analysis of the best available evidence in the light of our clinical experience. It is common in general practice to have to jump to quick decisions about diagnosis and therapy with incomplete information. Some GPs jump more quickly than others to more severe diagnoses and then to prescribing more drugs. The aim of the case study was to see which way you would go and then give you the opportunity to reflect on what may have influenced you to respond the way you did. The recommended diagnoses for Mrs Parker are: mild hypertension with mildly elevated cardiovascular disease (CVD) risk (not severe risk), life stage transition distress (not major depression) and normal introversion (not social phobia). You were asked to rate the appropriateness for Mrs Parker of 15 therapy options on a 1 to 5 scale where 1 = very inappropriate vs 5 = very appropriate. You were also asked questions designed to indicate your level of exposure to information from drug companies, e.g. "How often do you see drug reps?" Then you were asked questions designed to indicate your level of trust in information from drug companies, e.g. "What percentage of drug advertisements contain potentially misleading claims?" The results for 10 drug therapies are provided in this report. We plan to publish a more complete report later. The results show that the GPs who were more accepting of information from drug companies were more likely to believe that new drugs were appropriate for Mrs Parker. To demonstrate the importance of that finding three types of doctors are compared in this report: "Accepting GPs" vs "Majority GPs" vs "Sceptical GPs". "Accepting GPs" are those who indicated a belief that less than 50% of drug advertisements were potentially misleading and that their prescribing was improved by information from drug companies often or always. "Sceptical GPs" are those who indicated that more than 50% of drug advertisements were potentially misleading and that their prescribing was improved by information from drug companies rarely or never. "Majority GPs" are the remaining middle group between the Accepting and Sceptical GPs. "Majority GPs" indicated a belief that 50% of advertisements were potentially misleading and/or that their prescribing was improved by information from drug companies sometimes or gave a mix of "accepting" and "sceptical" answers. We received 1279 responses but the analysis presented here focuses on the 943 GPs who answered every question. Of those 943 GPs there were 95 Accepting GPs (10%), 759 Majority GPs (80.5%) and 89 Sceptical GPs (9.5%) Please find enclosed your response sheet so that, if you want to, you can compare your responses with responses from the 943 GPs and with our recommended answers.Appetite Suppressant
Results: 97% of all 943 GPs rated the Appetite Suppressant option as inappropriate or very inappropriate. GPs who believed that their prescribing is improved more often by information from drug companies were significantly more likely to rate the Appetite Suppressant option as more appropriate. (p=0.006)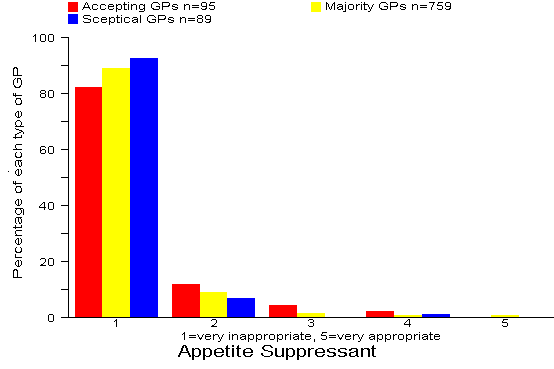 Comment:
Our recommended answer: 1 = very inappropriate.
There is no good evidence to support the use of appetite suppressants. Orlistat (Xenical ®) is not an appetite suppressant but deserves mention because it has been promoted heavily during 2000. Orlistat is not appropriate for Mrs Parker who is overweight but not obese (obese = BMI >30). Orlistat is an expensive way to lose a small amount of weight. There is no evidence yet on whether the loss is maintained long-term nor whether it leads to clinically important benefits.[1] It would be better for Mrs Parker to develop a taste for physical activity such as walking and a Mediterranean-like-diet such as the CSIRO / ACF 12345+ diet.
Comment:
Our recommended answer: 1 = very inappropriate.
There is no good evidence to support the use of appetite suppressants. Orlistat (Xenical ®) is not an appetite suppressant but deserves mention because it has been promoted heavily during 2000. Orlistat is not appropriate for Mrs Parker who is overweight but not obese (obese = BMI >30). Orlistat is an expensive way to lose a small amount of weight. There is no evidence yet on whether the loss is maintained long-term nor whether it leads to clinically important benefits.[1] It would be better for Mrs Parker to develop a taste for physical activity such as walking and a Mediterranean-like-diet such as the CSIRO / ACF 12345+ diet.
Thiazide
Results: There was more support for Thiazides than the other antihypertensive drug options. 30% of all 943 GPs rated the Thiazide option as appropriate or very appropriate. There were no significant differences between the three types of GP.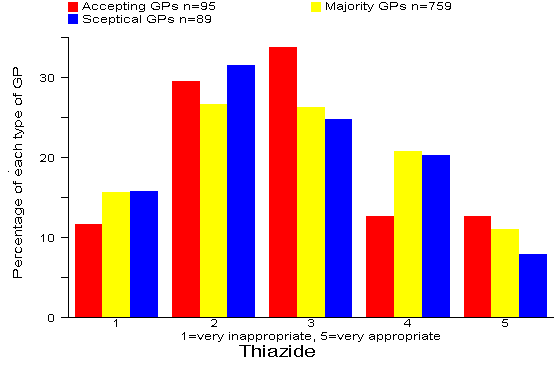 Comment:
Our recommended answer: 5 = very appropriate. However we assumed that non-drug therapy including walking and reduction of excessive salt had already commenced during the repeat visits required to make the diagnosis of hypertension. If you assumed that non-drug therapies had not been tried yet and consequently gave a lower rating for all antihypertensive drugs then we agree with you.
Thiazides and thiazide like drugs (eg chlorthalidone) are old but using them in very low doses (eg hydrochlorthiazide 25mg ½ tablet daily or chlorthalidone 25mg ½ tablet daily) is new. These drugs have been shown to delay cardiovascular disease and death for people like Mrs Parker. They are better supported by evidence than other antihypertensives. The best study comparing drugs for hypertension is the TOMHS study.[2] It compared chlorthalidone 15mg with an ACE inhibitor (enalapril), a calcium channel blocker (amlodipine), a beta-blocker (acebutolol, not available in Australia) and an alpha-blocker (doxazosin, not available in Australia). The TOMHS study found that chlorthalidone and acebutolol were best for improving quality of life. In our clinical experience, patients appreciate being able to pay less for a better drug.
Comment:
Our recommended answer: 5 = very appropriate. However we assumed that non-drug therapy including walking and reduction of excessive salt had already commenced during the repeat visits required to make the diagnosis of hypertension. If you assumed that non-drug therapies had not been tried yet and consequently gave a lower rating for all antihypertensive drugs then we agree with you.
Thiazides and thiazide like drugs (eg chlorthalidone) are old but using them in very low doses (eg hydrochlorthiazide 25mg ½ tablet daily or chlorthalidone 25mg ½ tablet daily) is new. These drugs have been shown to delay cardiovascular disease and death for people like Mrs Parker. They are better supported by evidence than other antihypertensives. The best study comparing drugs for hypertension is the TOMHS study.[2] It compared chlorthalidone 15mg with an ACE inhibitor (enalapril), a calcium channel blocker (amlodipine), a beta-blocker (acebutolol, not available in Australia) and an alpha-blocker (doxazosin, not available in Australia). The TOMHS study found that chlorthalidone and acebutolol were best for improving quality of life. In our clinical experience, patients appreciate being able to pay less for a better drug.
Calcium channel blocker (CCB)
Results: 44% of all 943 GPs rated the CCB option as inappropriate or very inappropriate. There were significant differences (p=0.004) between the three types of GP with 54% of Sceptical GPs rating the CCB option as inappropriate or very inappropriate.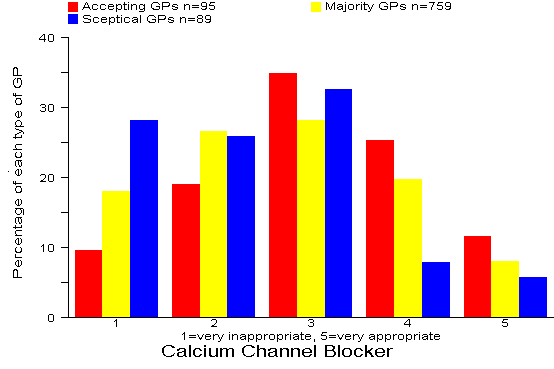 Comment:
Our recommended answer: 1 = very inappropriate.
There are two groups of CCBs.
The dihydropyridine CCB group includes amlodipine and felodipine. Most published trials comparing dihydropyridine CCBs with other antihypertensives have suggested that dihydropyridine CCBs may be associated with higher rates of cardiovascular events than thiazides and ACE inhibitors.[3] Consequently, we do not recommend dihydropyridine CCBs for hypertension.
Two trials have suggested that the non-dihydropyridine CCB verapamil and diltiazem may be as effective at reducing CVD events as the thiazides. Because there is no evidence of any clinically important advantage to justify the higher costs of non-dihydropyridine CCBs we do not recommend them for uncomplicated hypertension.
Comment:
Our recommended answer: 1 = very inappropriate.
There are two groups of CCBs.
The dihydropyridine CCB group includes amlodipine and felodipine. Most published trials comparing dihydropyridine CCBs with other antihypertensives have suggested that dihydropyridine CCBs may be associated with higher rates of cardiovascular events than thiazides and ACE inhibitors.[3] Consequently, we do not recommend dihydropyridine CCBs for hypertension.
Two trials have suggested that the non-dihydropyridine CCB verapamil and diltiazem may be as effective at reducing CVD events as the thiazides. Because there is no evidence of any clinically important advantage to justify the higher costs of non-dihydropyridine CCBs we do not recommend them for uncomplicated hypertension.
Angiotensin II receptor antagonists (A2 antagonist)
Results: 56% of all 943 GPs rated the A2 antagonist option as inappropriate or very inappropriate. There were significant differences (p<0.001) between the three types of GPs with 63% of Sceptical GPs rating the A2 antagonist option as inappropriate or very inappropriate.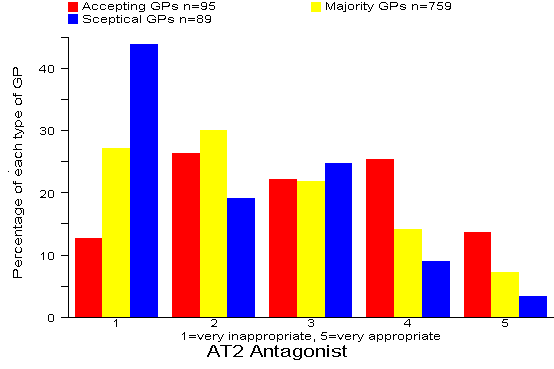 Comment:
Our recommended answer: 1 = very inappropriate.
A2 antagonists are very new drugs. They do reduce blood pressure. However, as yet there is no evidence of any clinically important benefit from lowering blood pressure with A2 antagonists so we do not recommend them. A2 antagonists may provide an alternative for those who require an ACE inhibitor, but who cannot tolerate it due to a drug-induced cough.
Comment:
Our recommended answer: 1 = very inappropriate.
A2 antagonists are very new drugs. They do reduce blood pressure. However, as yet there is no evidence of any clinically important benefit from lowering blood pressure with A2 antagonists so we do not recommend them. A2 antagonists may provide an alternative for those who require an ACE inhibitor, but who cannot tolerate it due to a drug-induced cough.
Hormone Replacement Therapy (HRT)
Results: 26% of all 943 GPs rated the HRT option as inappropriate or very inappropriate. There were no significant differences between the three types of GP.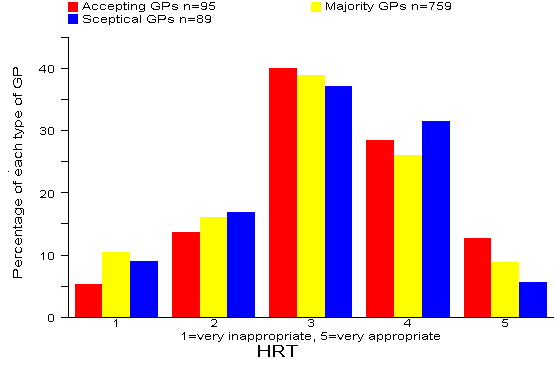 Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker does not have specific peri-menopausal symptoms so the issue here is the use of HRT for "prevention".
This is a difficult topic. Australian doctors have received conflicting messages about HRT. Most of these messages have been based on observational studies. Observational studies are less reliable than randomised controlled trials (RCTs). The best RCT done so far is the HERS study of secondary prevention for women with established cardiovascular disease. The HERS study found that HRT increases the rate of non-fatal infarcts and CVD deaths in the first year without providing any benefit over 5 years.[4]
In the absence of evidence of any benefit sufficient to compensate for short-term harm the use of HRT for secondary prevention is not justified. There is no RCT evidence to support the use of HRT in primary prevention. The harm to benefit ratios of drugs are usually worse for primary than for secondary prevention so it is difficult to justify use of HRT for Mrs Parker.[5]
Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker does not have specific peri-menopausal symptoms so the issue here is the use of HRT for "prevention".
This is a difficult topic. Australian doctors have received conflicting messages about HRT. Most of these messages have been based on observational studies. Observational studies are less reliable than randomised controlled trials (RCTs). The best RCT done so far is the HERS study of secondary prevention for women with established cardiovascular disease. The HERS study found that HRT increases the rate of non-fatal infarcts and CVD deaths in the first year without providing any benefit over 5 years.[4]
In the absence of evidence of any benefit sufficient to compensate for short-term harm the use of HRT for secondary prevention is not justified. There is no RCT evidence to support the use of HRT in primary prevention. The harm to benefit ratios of drugs are usually worse for primary than for secondary prevention so it is difficult to justify use of HRT for Mrs Parker.[5]
Statin
Results: 60% of all 943 GPs rated the Statin option as inappropriate or very inappropriate. There were significant differences (p=0.01) between the three types of GP with 77% of Sceptical GPs rating the Statin option as inappropriate or very inappropriate.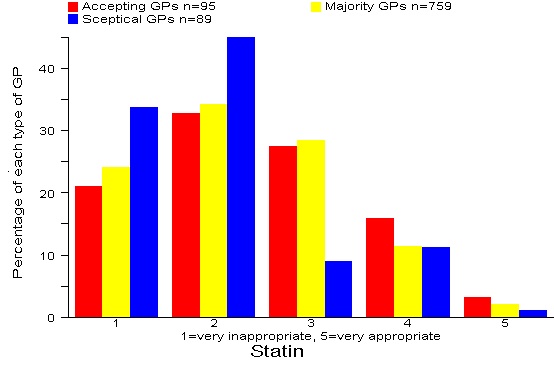 Comment:
Our recommended answer: 1 = very inappropriate.
We recommend the New Zealand CVD risk calculator distributed by NPS and also available on the British Medical Journal website.[6] This calculator makes it easy to estimate that once her blood pressure is addressed, Mrs Parker’s absolute risk of having any cardiovascular problems in the next 5 years is likely to be less than 5%.
Because Mrs Parker has such a low risk her chances of getting a worthwhile benefit from a statin are tiny. The benefit that could be gained from a statin is very likely to be so small that the risks of adverse effects are not justified, let alone the cost. Use of drugs in situations where they are not cost effective diverts resources from people who need those resources more. Improvements in diet and physical activity levels would be more appropriate.
Comment:
Our recommended answer: 1 = very inappropriate.
We recommend the New Zealand CVD risk calculator distributed by NPS and also available on the British Medical Journal website.[6] This calculator makes it easy to estimate that once her blood pressure is addressed, Mrs Parker’s absolute risk of having any cardiovascular problems in the next 5 years is likely to be less than 5%.
Because Mrs Parker has such a low risk her chances of getting a worthwhile benefit from a statin are tiny. The benefit that could be gained from a statin is very likely to be so small that the risks of adverse effects are not justified, let alone the cost. Use of drugs in situations where they are not cost effective diverts resources from people who need those resources more. Improvements in diet and physical activity levels would be more appropriate.
Benzodiazepine
Results: 90% of all 943 GPs rated the Benzodiazepine option as inappropriate or very inappropriate. GPs who believed that their prescribing is improved more often by information from drug companies were significantly more likely to rate the Benzodiazepine option as more appropriate. (p=0.003)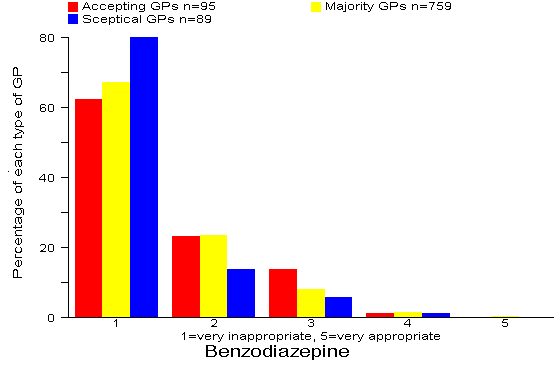 Comment:
Our recommended answer: 1 = very inappropriate.
A recent meta-analysis has found that whilst benzodiazepine users think that they get to sleep 10 to 20 minutes quicker than with placebo the objective difference in getting to sleep is not significant.[7] The average decrease in sleep latency was only 4.2 minutes (95% confidence intervals –0.7 to 9.2 minutes).
It is difficult to justify the initiation of benzodiazepines because the benefits are so small, there are risks of cognitive dysfunction and addiction and there are non-drug therapies for insomnia that work better. It would be better to address the causes of Mrs Parker’s insomnia.
Comment:
Our recommended answer: 1 = very inappropriate.
A recent meta-analysis has found that whilst benzodiazepine users think that they get to sleep 10 to 20 minutes quicker than with placebo the objective difference in getting to sleep is not significant.[7] The average decrease in sleep latency was only 4.2 minutes (95% confidence intervals –0.7 to 9.2 minutes).
It is difficult to justify the initiation of benzodiazepines because the benefits are so small, there are risks of cognitive dysfunction and addiction and there are non-drug therapies for insomnia that work better. It would be better to address the causes of Mrs Parker’s insomnia.
Tricyclic antidepressant (TCA)
Results: 63% of all 943 GPs rated the TCA option as inappropriate or very inappropriate. There were no significant differences between the three types of GP.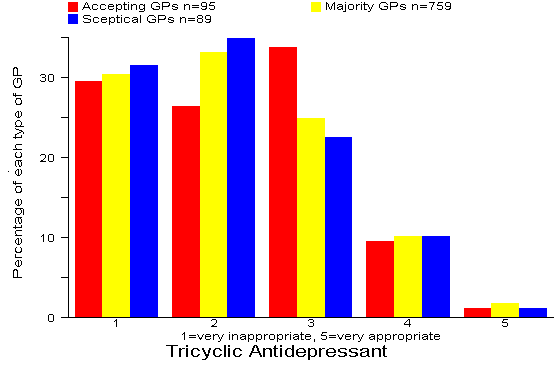 Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker has life stage transition distress. She does not meet the diagnostic criteria for major depression. If she did have major depression severe enough to require hospitalisation then a TCA would have been better than an SSRI because there is some evidence TCAs are more effective. For less severe depression there is no clear difference in the effectiveness of TCAs and SSRIs. This may be because most people get better anyway or because of the placebo effect. The rate of discontinuations because of side effects for SSRIs and secondary amine TCAs such as desipramine (Pertofran®) are not different. When considering what to prescribe, when there is no clear evidence of a difference in effectiveness, it may be useful to mention the adverse effects of the alternatives and ask patients about their preferences (e.g. dry mouth vs sexual dysfunction). TCAs are more dangerous in overdose. Unfortunately there is no good evidence that the increased use of SSRIs has reduced the rate of fatal suicides from all causes.
Cognitive Behaviour Therapy (CBT) is as effective as drugs for major depression in the short term and leads to lower relapse rates. CBT is more appropriate, compared to drugs, for less severe depression and distress. For more on depression see the next section.
Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker has life stage transition distress. She does not meet the diagnostic criteria for major depression. If she did have major depression severe enough to require hospitalisation then a TCA would have been better than an SSRI because there is some evidence TCAs are more effective. For less severe depression there is no clear difference in the effectiveness of TCAs and SSRIs. This may be because most people get better anyway or because of the placebo effect. The rate of discontinuations because of side effects for SSRIs and secondary amine TCAs such as desipramine (Pertofran®) are not different. When considering what to prescribe, when there is no clear evidence of a difference in effectiveness, it may be useful to mention the adverse effects of the alternatives and ask patients about their preferences (e.g. dry mouth vs sexual dysfunction). TCAs are more dangerous in overdose. Unfortunately there is no good evidence that the increased use of SSRIs has reduced the rate of fatal suicides from all causes.
Cognitive Behaviour Therapy (CBT) is as effective as drugs for major depression in the short term and leads to lower relapse rates. CBT is more appropriate, compared to drugs, for less severe depression and distress. For more on depression see the next section.
SSRI for depression
Results: 23% of all 943 GPs rated the SSRI for depression option as inappropriate or very inappropriate. There were significant differences (p=0.028) between the three types of GP with 37% of Sceptical GPs rating the SSRI for depression option as inappropriate or very inappropriate.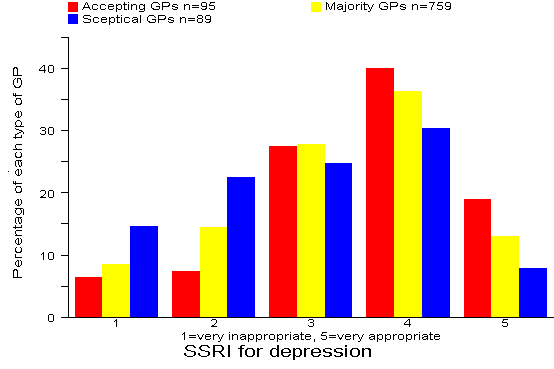 Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker is distressed. That is different from depression. However, we accept that some GPs may have interpreted the question as indicating that the diagnosis of depression had been made. Mrs Parker is likely to find new meaning in life by herself. However a few half hour sessions of simplified cognitive therapy could be dramatically helpful. Clinical experience suggests that use of any antidepressant risks masking her symptoms and undermining her ability to achieve mastery over the cause of her distress. One way to learn about simplified cognitive therapy is to read Greenberger D, Padesky C. Mind over mood. Guilford Press, New York 1995. Clinical experience suggests that it is easier to learn how to provide simplified cognitive therapy than many GPs realise.
Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker is distressed. That is different from depression. However, we accept that some GPs may have interpreted the question as indicating that the diagnosis of depression had been made. Mrs Parker is likely to find new meaning in life by herself. However a few half hour sessions of simplified cognitive therapy could be dramatically helpful. Clinical experience suggests that use of any antidepressant risks masking her symptoms and undermining her ability to achieve mastery over the cause of her distress. One way to learn about simplified cognitive therapy is to read Greenberger D, Padesky C. Mind over mood. Guilford Press, New York 1995. Clinical experience suggests that it is easier to learn how to provide simplified cognitive therapy than many GPs realise.
SSRI for social phobia
Results: 35% of all 943 GPs rated the SSRI for social option as inappropriate or very inappropriate. There were significant differences (p=0.008) between the three types of GP with 48% of Sceptical GPs rating the SSRI for social phobia option as inappropriate or very inappropriate.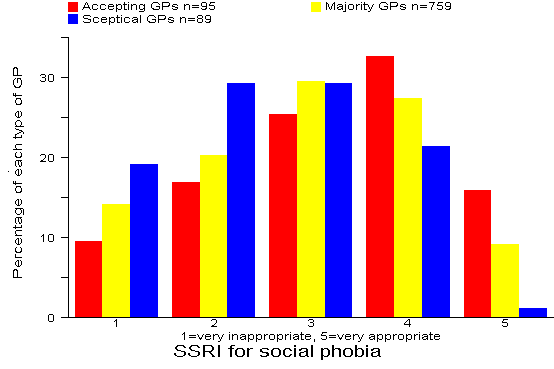 Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker does not meet the diagnostic criteria for social phobia. However, we accept that some GPs may have interpreted that question as indicating that the diagnosis of social phobia had been made.
Mrs Parker is one of 40% of the Australian population who are introverts. Introversion is a normal personality variant. It would be appropriate to tell her that her anxiety about parties is normal and arises from a personality variation which also brings many advantages both for her and for those she cares about (eg capacity for depth of focus). It would also be appropriate to tell her that mild anxiety improves performance and so whilst it is often unpleasant it can be beneficial.
It would not be appropriate to medicalize 40% of the Australian population.
Comment:
Our recommended answer: 1 = very inappropriate.
Mrs Parker does not meet the diagnostic criteria for social phobia. However, we accept that some GPs may have interpreted that question as indicating that the diagnosis of social phobia had been made.
Mrs Parker is one of 40% of the Australian population who are introverts. Introversion is a normal personality variant. It would be appropriate to tell her that her anxiety about parties is normal and arises from a personality variation which also brings many advantages both for her and for those she cares about (eg capacity for depth of focus). It would also be appropriate to tell her that mild anxiety improves performance and so whilst it is often unpleasant it can be beneficial.
It would not be appropriate to medicalize 40% of the Australian population.
[1] Therapeutics Letter 34 www.ti.ubc.ca/pages/letter34.htm#Orlistat
[2] Grimm RH. Relationships of quality-of-life measures to long-term lifestyle and drug treatment in the Treatment of Mild Hypertension Study. Arch Intern Med. 1997;157(6):638-48
[3] Healthy Scepticism Jan 1999, Vol 2 (1) www.healthyskepticism.org/nz/healthy.htm
[4] Hulley et al. Randomized trial of estrogen plus progesterone for secondary prevention of coronary heart disease in postmenopausal women. JAMA 1998;280:7:605-13
[5] Therapeutics Letter 30 www.ti.ubc.ca/pages/letter30.htm
Page views since 15 March 2010: 101489
Comments
Our members can see and make comments on this page.
















